Long Covid-19 and Yoga Therapy
A simple truth
Let’s start with one simple truth.
While for many of us it feels like we’ve been in this state of flux for far too long already, it is early days and it will be a long time before Covid-19 is fully understood.
Both mainstream Western medicine and complimentary medicine are working tirelessly supporting those with both acute Covid-19 and post-acute Covid-19, also known as Long Covid-19. In many cases, such as the Seacole Centre in Surrey, they are coming together in recognition that we are complex humans with wide ranging and often unique needs even for the same condition.
What is Long Covid-19?
Definition
An expert online panel hosted by the British Medical Journal (BMJ) defined long Covid-19 as “not recovering [for] several weeks or months following the start of symptoms that were suggestive of Covid, whether you were tested or not” [efn_note]British Medical Journal : Long Covid: How to define it and how to manage it. https://www.bmj.com/content/370/bmj.m3489[/efn_note]
“not recovering [for] several weeks or months following the start of symptoms that were suggestive of Covid, whether you were tested or not” 1
A separate BMJ article goes further and breaks long Covid-19 down into two categories, post-acute Covid -19, defined as extending beyond three weeks from the onset of first symptoms and chronic Covid-19 which extends beyond 12 weeks. [efn_note]British Medical Journal : Management of post-acute covid-19 in primary care : https://www.bmj.com/content/370/bmj.m3026[/efn_note]
Symptoms
One study in Italy of 143 patients published in the Journal of the American Medical Association and cited in the BBC article ‘Long Covid: Why are some people not recovering’ tracked patients who had been in hospital for a period of one month after being discharged. The distribution of symptoms for that cohort is shown below. This particular cohort was acute enough to need hospitalisation and was followed for only one month post release, however the symptoms mirror other emerging accounts from those suffering.
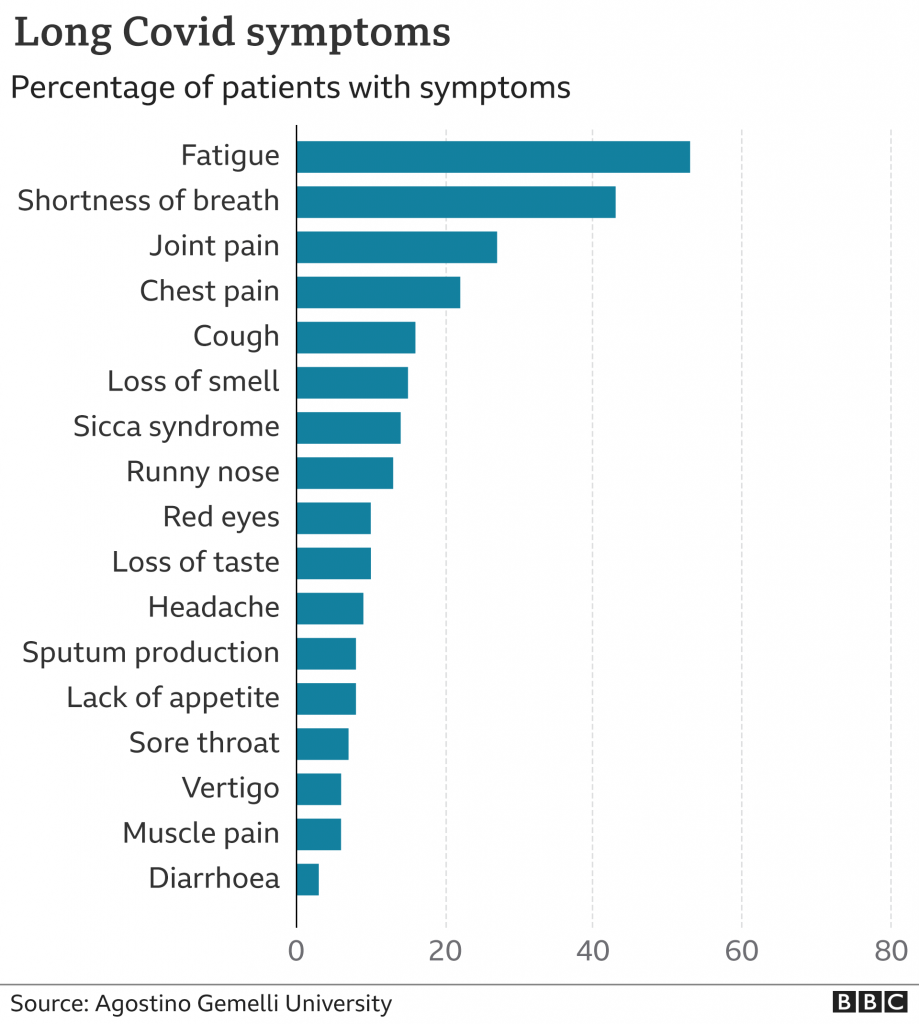
The above chart was sourced from Agostino Gemelli University as is shown in the BBC article ‘Long Covid: Why are some people no recovering?
Wider Systemic Effects
This is not an exhaustive list of symptoms and evidence is emerging that covid-19 can have wider effects on a multitude of organs and systems in our body, including heart, lungs, kidneys and the gut.1, 2
If you are suffering from Long Covid-19 and experiencing any symptoms that may indicate more severe respiratory, cardiovascular or neurological conditions please see your doctor.
Impact on Mental Health
The impact goes far beyond the physical with potentially profound impacts on mental health for those suffering with Long Covid-19 and for those supporting them.
In my private yoga therapy work the top two mental health impacts seen with Long Covid-19 cases have been anxiety and depressed mood (or situational depression).
Anxiety
Wondering when the next relapse will come, being concerned that they may by contagious to those around them and being afraid to see people, worrying about their ability to work, earn an income and provide for themselves and their families.
Depressed Mood or Situational Depression
There is often a feeling of hopelessness, a sense of lack of control, and in some instances not feeling heard, seen or believed that their condition and experience is real.
If you are suffering from anxiety, depression or any other mental health challenge and do not feel like you are coping or you do not have a strong support system in place or simply want to get reassurance that you are ok or need someone to speak to please do reach out to a support line or resource such as Mind, Samaritans or look for mental health services in your area.
Who Does Long Covid Affect?
Data
Real Stories
Statistics and numbers are invaluable to the big picture, but stories are powerful insights into felt experience and the soul residing beneath this data.
Most major news outlets have run at least one story on Long Covid-19, with stark insights into the experiences of those who have been navigating this uncertain condition and state of being.
In a BBC[efn_note]BBC News : Long Covid: My fatigue was like nothing I’ve experienced before. https://www.bbc.co.uk/news/stories-54106272[/efn_note] highlight piece we met Jade, who went from being a vibrant 32 year old with a fulfilling job working with young people from disadvantaged backgrounds, a busy social life and exercising 3 times per week to sleeping 16 hours a day, suffering dizzy spells, fainting and struggling to carry out basic activities of daily living. She described her fatigue “like nothing I’ve experienced before”.
For this and other first-hand accounts head over to these stories on the BBC6, Guardian[efn_note]The Guardian : Brain fog, phantom smells and tinnitus: my experience as a Covid ‘long hauler’ : https://www.theguardian.com/commentisfree/2020/aug/05/brain-fog-phantom-smells-and-tinnitus-my-experience-as-a-covid-long-hauler[/efn_note] and Telegraph[efn_note]The Telegraph : I had to leave the nursing job I love because of long-covid. https://www.telegraph.co.uk/health-fitness/mind/had-leave-nursing-job-love-long-covid/[/efn_note].
Can Yoga Therapy Help?
In short, yes yoga therapy has great potential to help.
However, like many therapies, both mainstream and complimentary, there is no one size fits all and a portion of the effect comes from engaging positively with your therapy of choice and your relationship with the therapist.
Yoga is a non-invasive therapy that can affect physical, mental, emotional and spiritual change. If done with a knowledgeable and experienced practitioner it is safe and can greatly improve the mind-body-emotion connection.
If yoga is an avenue you are keen to explore, here as some of the ways that it has been shown to help with some of the symptoms that we are now seeing in Long Covid-19.
While these studies are not specific to Long Covid-19 there is the potential that similar benefits could be reached.
Reducing Persistent Fatigue
A 2011 study published in eCAM showed yoga to be an effective intervention in reducing chronic fatigue in breast cancer survivors.
The primary outcome was subjective fatigue with a secondary outcome measured under the vitality scale of SF-36, a quality of life survey widely used and accepted in clinical research. Both measured outcomes saw statistically significant improvements in scores over the course of the study. In addition evidence also showed that these improvements persisted over the 3 month post-intervention follow-up.[efn_note]Julienne E. Bower, Deborah Garet, Beth Sternlieb, “Yoga for Persistent Fatigue in Breast Cancer Survivors: Results of a Pilot Study”, Evidence-Based Complementary and Alternative Medicine, vol. 2011, Article ID 623168, 8 pages, 2011. https://doi.org/10.1155/2011/623168[/efn_note]
One study found that yoga showed greater improvement in mood, greater reductions in anxiety and increased GABA activity which is correlated with mood and anxiety disorders.[efn_note]Chris C. Streeter, Theodore H. Whitfield, Liz Owen, Tasha Rein, Surya K. Karri, Aleksandra Yakhkind, Ruth Perlmutter, Andrew Prescot, Perry F. Renshaw, Domenic A. Ciraulo, and J. Eric Jensen.The Journal of Alternative and Complementary Medicine.Nov 2010.1145-1152.http://doi.org/10.1089/acm.2010.0007[/efn_note]
Improved Respiratory Function
A 2011 study published in the BMJ Journals found that yoga training may be beneficial in improving respiratory function and sympathovagal balance in a healthy elderly population.[efn_note]Santaella DF, Devesa CRS, Rojo MR, et al Yoga respiratory training improves respiratory function and cardiac sympathovagal balance in elderly subjects: a randomised controlled trial. BMJ Open 2011;1:e000085. doi: 10.1136/bmjopen-2011-000085[/efn_note] Sympathovagal balance refers to the autonomic nervous systems ability to balance between the fight and flight and the rest and digest states in a healthy manner.
In short, specific yogic breathing techniques were found to have a positive impact on both respiratory function and on the nervous system’s ability to self-regulate.
Stress Management
Blood pressure is a key indicator of our stress levels and yoga has been found to be able to directly impact our blood pressure. A 2008 study looking at the impact of three types of breath work all involving manipulation of the breath through traditional yoga practices found that these techniques could increase, decrease and stabilise blood pressure and improve Heart Rate Variability (HRV). The authors of the study suggested that using yoga breath techniques had potential therapeutic uses.[efn_note]Raghuraj, P., Telles, S. Immediate Effect of Specific Nostril Manipulating Yoga Breathing Practices on Autonomic and Respiratory Variables. Appl Psychophysiol Biofeedback 33, 65–75 (2008). https://doi.org/10.1007/s10484-008-9055-0[/efn_note]
Reducing Anxiety
Yoga plays a role in hormone regulation and has been shown by various studies to reduce cortisol levels. Reducing cortisol levels is linked to reducing perceived stress, reducing anxiety and improving general feelings of wellbeing.[efn_note]McCall MC (2013) How Might Yoga Work? An Overview of Potential Underlying Mechanisms. J Yoga Phys Ther 3: 130. doi:10.4172/2157- 7595.1000130[/efn_note]
One study found that yoga showed greater improvement in mood, greater reductions in anxiety and increased GABA activity which is correlated with mood and anxiety disorders.[efn_note]Chris C. Streeter, Theodore H. Whitfield, Liz Owen, Tasha Rein, Surya K. Karri, Aleksandra Yakhkind, Ruth Perlmutter, Andrew Prescot, Perry F. Renshaw, Domenic A. Ciraulo, and J. Eric Jensen.The Journal of Alternative and Complementary Medicine.Nov 2010.1145-1152.http://doi.org/10.1089/acm.2010.0007[/efn_note]